Medicare Going In 'Right Direction' On Opioid Epidemic

Prescriptions for 2 drugs accustomed to treat opioid addiction increased significantly from 2021 to 2021 for individuals on Medicare, according to a federal report out Wednesday.
About 174,000 Medicare beneficiaries received such a medication – either buprenorphine or naltrexone – to help them with recovery in 2021, based on the Office of Inspector General within the Department of Health and Human Services.
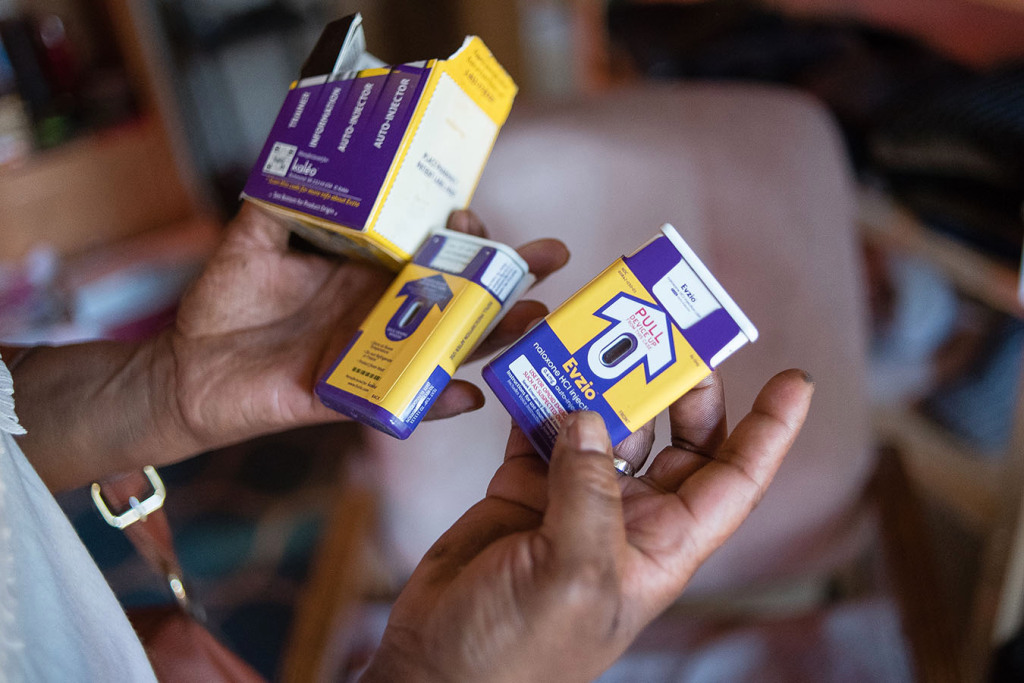
In addition, prescriptions for naloxone, the drug that may reverse an opioid overdose, spiked since 2021, rising 501% ― and that's likely an underestimate since it doesn't include doses from the nasal spray Medicare members might have received through local programs, the OIG said.
“For now, the numbers 're going in the right direction,” said Miriam Anderson, lead investigator on the report. “But this is a national crisis and that we must remain vigilant and continue to fight this epidemic and ensure that opioids are prescribed and used appropriately.”
During the 2 years studied, the threat of recent addictions appeared to slow. Prescriptions for an opioid through Medicare Part D decreased by 11%. The numbers of the beneficiaries considered at serious risk for misuse or overdose ― either because they received extreme levels of opioids or appeared to be “doctor shopping” ― dropped 46%. And there were 51% fewer doctors or other providers flagged for prescribing opioids to patients at serious risk from 2021 through 2021.
The report says the OIG along with other law enforcement agencies will investigate highest-level prescribers for possible fraud and signs that some providers operate pill mills. The report mentions a health care provider in Florida who provided 104 high-risk Medicare patients with 2,619 opioid prescriptions.
It will be up to Medicare to follow along with up with patients whose opioid use suggests addiction, recreational use or resale. Once, a Pennsylvania woman received 10,728 oxycodone pills and 570 fentanyl patches from a single physician during 2021. A Medicare member in Alabama acquired 56 opioid prescriptions from 25 different prescribers within twelve months.
In an argument, the Centers for Medicare & Medicaid Services said: “Fighting the opioid epidemic is a top priority for the Trump administration. We are encouraged through the OIG's conclusion which finds significant progress has been created in our efforts to lower opioid misuse while simultaneously increasing medication assisted treatment in the Medicare Part D program.”
The agency points to recent efforts to curb opioid misuse together with a seven-day limit on first-time opioid prescriptions, pharmacy alerts about Medicare beneficiaries who receive high doses of pain meds and drug management programs that may restrict a patient's supply. CMS says it doesn't make use of a “one size fits all” approach. Medicare patients in long-term care facilities or hospice care and people in cancer treatment are exempt from the opioid-prescribing restrictions.
The opioid-prescribing limits are raising alarms among some Medicare recipients, especially those who qualify based on a long-term disability and cope with severe, chronic pain.
Jae Kennedy, a disability policy expert at Washington State University, said reducing opioid prescriptions is generally a good development.
“But we hear from people in the disability community who feel like they're being victimized with this new, very stringent set of dispensing limits,” said Kennedy. “People have been managing their pain, in some instances for several years without a problem, and today they're being type of criminalized by this new bureaucratic backlash.”
Anderson said the OIG agrees that “some patients need opioids and they should receive those required for their condition. This report raises concerns that some patients might be receiving opioids far above those needs.”
While most Medicare beneficiaries are 65 or older, the 15% who are under 65 and disabled could be the key bit of this report. Kennedy's research shows they are up to 3 times more prone to describe persistent pain than are also adults and 50% more likely to report opioid misuse. A 2021 OIG report discovered that 74% of Medicare beneficiaries at serious risk for addiction and overdose deaths were under age 65.
Kennedy said it is good to determine Medicare expanding access to medication assisted treatment, referred to as MAT, for addiction, but the agency needs to ensure that more buprenorphine prescribers accept all patients, not just the ones who are easiest to manage. Patients with disabilities often need many different medications for multiple mental and physical health conditions.
“Saying, 'Well, because you've got schizophrenia or manic depressive disorder, we can't treat you,' I think is discriminatory,” Kennedy said. “It's happening with private buprenorphine prescribers within this country since there are very few.”
Americans 65 or older have the lowest rates of opioid overdose deaths. Nevertheless, the CDC says the amount of deaths among seniors increased by 279% from 1999 to 2021.

